The ABC’s of Toileting Readiness for Kindergarten!
The ABC’s of Toileting Readiness for Kindergarten!
Kindergarten is a time filled with excitement and anticipation, but also marked by apprehension and changes in routine. Amidst this whirlwind of new experiences, one aspect that often proves challenging is toileting readiness. Feeling apprehensive about your kindergartener’s bathroom autonomy at school is entirely natural. Mastering the skills required can be daunting, especially for those encountering hurdles along the way. Achieving toileting success in kindergarten is a milestone for both children and their caregivers.
Here are some factors that contribute to kindergarten toileting success:
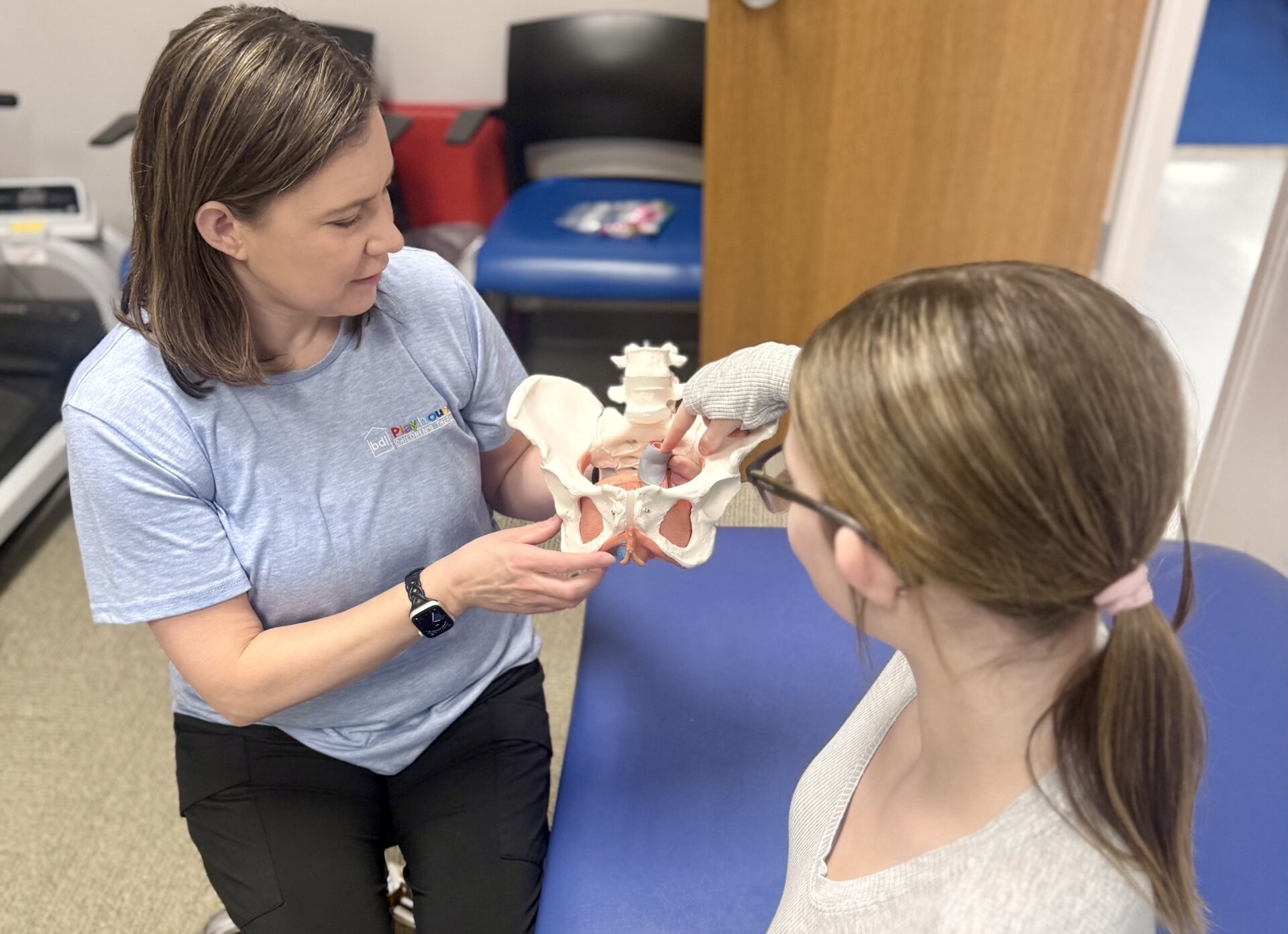
- Awareness of bodily functions: This is called interoception, an important part of our sensory system. It allows your child to recognize when they need to use the bathroom, whether it’s for urination or bowel movements.
- Communication with caregivers: The ability for your child to signal when they need to use the toilet and when they’ve had accidents.
- Comfort with the bathroom environment: Being at ease with the sights, sounds, and smells of the bathroom is essential for successful toileting.
- Understands toileting sequence: Knowing the steps involved in using the toilet, from undressing, sitting or standing, wiping, dressing, and washing hands with minimal assistance.
- Independence on child-size toilet: Being able to get on and off the toilet seat without help and maintaining balance for a few minutes.
- Comfort using bathrooms outside home: Transitioning to using toilets in unfamiliar settings, like at school.
- Self-care skills: Pulling up and down pants and underwear and attempting to wipe independently with minimal assistance.
It’s helpful to remember that toileting success is a developmental milestone, and every child progresses at their own pace. While some children may quickly adapt to kindergarten toileting routines, others may require additional time and support.
If your child needs extra assistance to prepare for kindergarten success, don’t hesitate to contact us. Our experienced therapists specialize in addressing toileting challenges, including avoidance, withholding, constipation management, and daytime and nighttime incontinence. With personalized interventions and compassionate support, we’re here to help your child navigate this important milestone with confidence.
Written By: Andrea Turnell, DPT and Dana Bukala, PTA