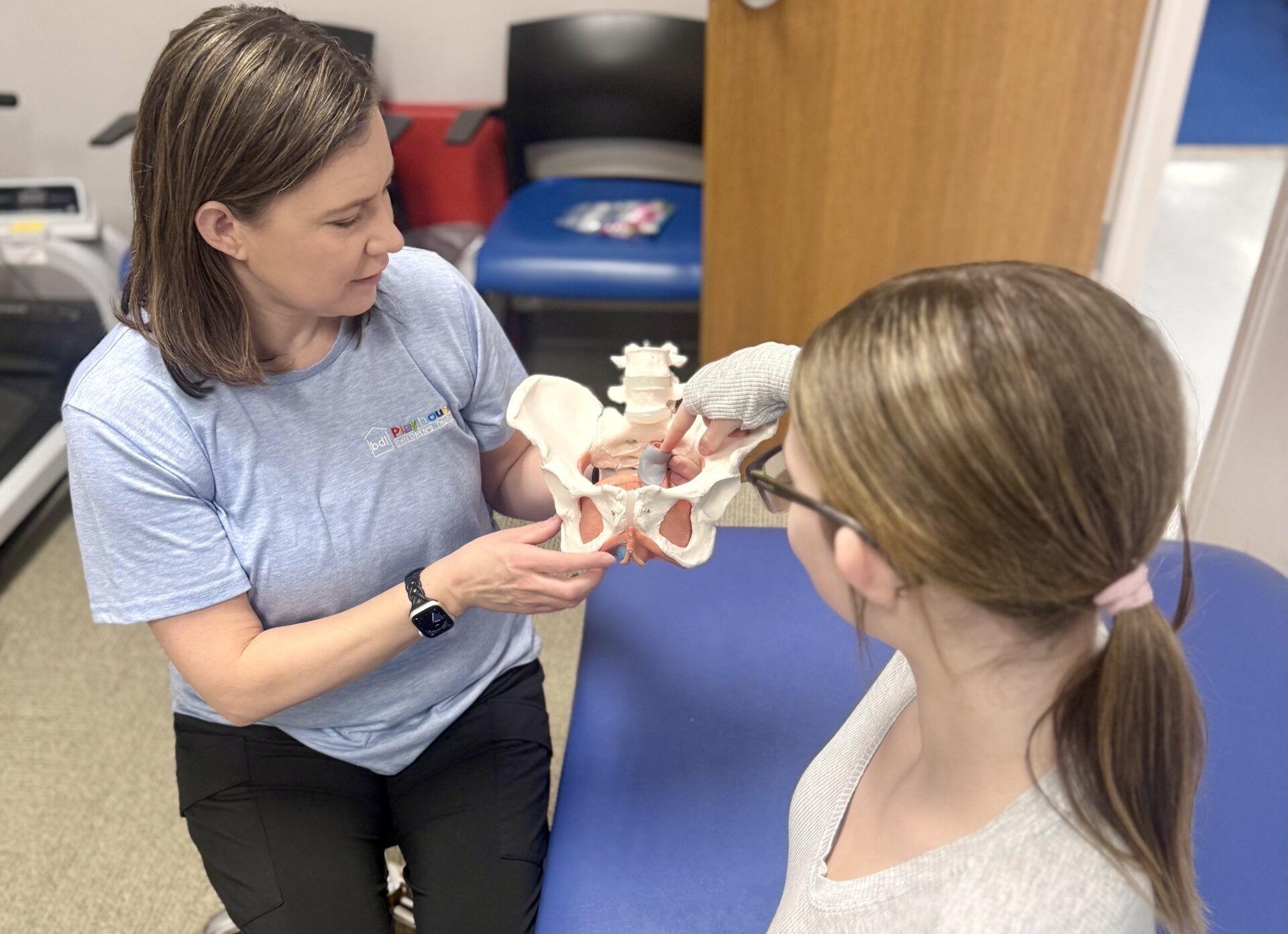
Constipation and Bedwetting: How Physical Therapy Can Help
Bedwetting is stressful for kids and parents alike, and it often feels like you’ve tried everything—limiting fluids, nighttime reminders, or alarms—with limited results. You may have even heard that they will outgrow it. One of the most overlooked contributors is constipation, and one of the most effective ways to address it is through pediatric pelvic floor physical therapy.
Understanding the connection between constipation and bladder function can empower families and open the door to meaningful improvements.
Why Constipation Matters for Bedwetting
The rectum (where stool is stored) sits directly behind the bladder. When a child is constipated:
1. Stool Takes Up Space and Pushes on the Bladder
A full rectum puts pressure on the bladder, reducing how much urine it can hold comfortably. This makes nighttime accidents more likely—especially during deep sleep.
2. The Nerves Become Confused
Chronic constipation can stretch the rectum, affecting the nerves that communicate with the bladder. Kids may not feel bladder fullness or may get mixed signals that lead to urgency or accidents.
3. The Pelvic Floor Has to Work Harder
The pelvic floor muscles help children hold in urine and regulate bowel movements. When constipation is present, these muscles often become tense, weak, or poorly coordinated—directly impacting continence during the day and night.
The Physical Therapy Perspective
Pediatric physical therapists look at constipation and bedwetting from a whole-body viewpoint. We consider:
- Pelvic floor strength and coordination
- Breathing patterns that influence pressure on the bladder
- Posture during toileting and daily activities
- Movement habits that contribute to holding behaviors
- Nervous system regulation, especially in sensory-sensitive kids
Bedwetting is rarely just a “bladder problem”—it is often a muscle coordination and biomechanics issue that PT can address.
How Physical Therapy Helps With Constipation and Bedwetting
1. Pelvic Floor Muscle Training
Children are taught—through play, games, and biofeedback when appropriate—how to relax the pelvic floor to poop effectively and contract it to maintain bladder control. Many kids with constipation unknowingly over-tighten these muscles, which worsens both constipation and bedwetting.
Pelvic floor biofeedback is a gentle, kid-friendly tool used in pediatric physical therapy to help children understand how their pelvic floor muscles work. Small stickers are placed on the skin (not inside the body) connected to a computer that turns muscle activity into simple pictures or games. As the child watches the screen, they can see when their muscles are tightening or relaxing, which helps them learn how to use these muscles the right way for easier toileting. It’s safe, comfortable, and often feels more like playing a game than doing an exercise.
2. Improving Toilet Posture
Appropriate toilet posture can make pooping easier and help empty the bladder more fully. PTs help families improve core stability and help set up a bathroom routine with:
- A footstool for stability
- Proper trunk alignment
- Breathing cues to reduce straining
3. Addressing Breath Coordination
Holding breath during bowel movements or other activities increases abdominal pressure and disrupts pelvic floor control. PTs help kids learn diaphragmatic breathing to support both bowel and bladder function.
4. Increasing Core and Postural Strength
Weakness in the core or hips can make it harder for children to maintain pelvic stability. Strengthening helps improve the effectiveness of pelvic floor muscles.
5. Establishing Healthy Habits
Therapists work on routines to help support healthier bowel movements and bladder emptying:
- Timed voiding
- Relaxed toilet sits after meals
- Recognizing body signals
- Reducing withholding behaviors
6. Sensory & Behavioral Strategies
For children with sensory needs, toileting refusal or avoidance, ADHD, or autism, PT can help modify routines and environments so bathroom tasks feel safer and more predictable. PTs often collaborate with counselors, OT, and speech therapists to help best support their goals.
Signs Your Child May Benefit From Physical Therapy
Consider a PT evaluation if your child has:
- Bedwetting after age 6
- Hard, infrequent, or painful bowel movements
- Stool accidents or frequent skid marks
- Urinary urgency, frequency, or daytime accidents
- Sensory challenges around toileting
- Poor posture or difficulty relaxing to poop
- A history of constipation that keeps returning
Addressing this early helps prevent chronic stretching of the rectum and long-term bladder dysfunction.
The Good News: Real Improvements Are Possible
Many families are surprised at how quickly things improve once constipation and pelvic floor coordination are addressed. Some families even notice improvements after the initial evaluation. The typical treatment duration is 8-12 sessions with families participating in home exercise progreams.
Reducing stool buildup creates more space for the bladder, improves nerve signaling, and allows the pelvic floor to function properly. As bowel movements normalize and the bladder empties more effectively, nighttime dryness often follows.
Physical therapy provides children with the tools, awareness, and body confidence they need to support healthy bowel and bladder habits. With time and consistency, kids can achieve better control, sleep more comfortably, and participate fully in daily life without embarrassment.